What Does Optimal Prenatal Health Look Like and How Can I Achieve It?
Achieving optimal prenatal health requires a comprehensive approach that combines medical supervision, nutritional support, and lifestyle modifications. Pregnancy is a critical period where maternal choices directly impact fetal development, making it essential to understand the key components of evidence-based prenatal care.
The foundation of optimal prenatal health starts before conception and continues throughout all three trimesters. Working with qualified healthcare providers and following established guidelines significantly improves outcomes for both mother and baby.
What Are the Essential Prenatal Vitamins and Nutrients Needed During Pregnancy?
Folic acid is particularly important during the first trimester, as it reduces the risk of neural tube defects by up to 70%. Iron prevents maternal anemia and ensures adequate oxygen delivery to the fetus. Calcium supports fetal bone development and helps maintain maternal bone health. DHA (docosahexaenoic acid), an omega-3 fatty acid, supports fetal brain and eye development. Starting prenatal vitamins before conception provides optimal protection.
What Prenatal Screening Tests and Appointments Are Recommended at Each Trimester?
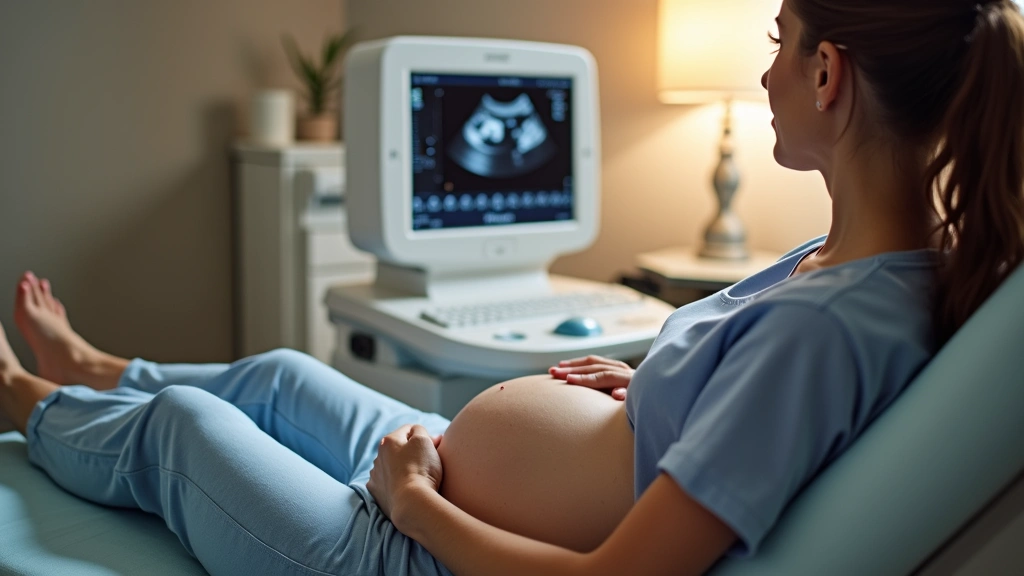
The first trimester dating ultrasound confirms pregnancy viability and establishes accurate due dates. Second trimester screening detects chromosomal abnormalities and anatomical issues. The glucose tolerance test screens for gestational diabetes around 24-28 weeks. Third trimester visits monitor blood pressure, fetal growth, and positioning. According to ACOG guidelines, these visits become more frequent as delivery approaches to catch complications early.

How Does Exercise and Nutrition Impact Prenatal Health Outcomes?
Most pregnant women should aim for 150 minutes of moderate-intensity aerobic activity weekly, such as brisk walking or swimming. Proper nutrition means consuming an additional 300-500 calories daily during the second and third trimesters, focusing on lean proteins, whole grains, fruits, and vegetables. Adequate hydration and consistent meal timing help maintain stable blood sugar and energy levels.
What Lifestyle Factors and Substances Should Be Avoided During Pregnancy?
Alcohol consumption during pregnancy increases the risk of fetal alcohol spectrum disorders. Smoking reduces oxygen to the fetus and increases miscarriage risk. Stress management through meditation, yoga, or counseling supports both maternal and fetal health. Aim for 7-9 hours of quality sleep nightly to support immune function and emotional wellbeing.

Can Telehealth Be Used for Prenatal Care and What Are Its Limitations?
Virtual visits offer convenience for discussing symptoms, reviewing lab results, and receiving medical advice, but cannot replace critical in-person assessments. Remote patient monitoring devices can track vital signs between visits, enhancing safety.
What Are Common Prenatal Health Risks and How Are They Managed?
Gestational diabetes affects 2-10% of pregnancies and is managed through glucose monitoring and dietary changes. Preeclampsia, characterized by high blood pressure and protein in urine, requires close monitoring and may necessitate early delivery. Regular screening identifies these conditions early, allowing for timely intervention and improved outcomes.
How Do I Find and Select an Optimal Prenatal Care Provider or Program?
Board-certified obstetricians and certified nurse midwives both provide excellent prenatal care. Consider whether you prefer a digital health component for convenience. Interview potential providers about their approach to wellness during pregnancy and their availability for urgent concerns.
Frequently Asked Questions
When should I start prenatal care?
Early prenatal care allows providers to identify risk factors, initiate appropriate supplementation, and establish baseline health metrics for comparison throughout pregnancy.
Is it normal to have anxiety about prenatal health?
Mental health support is an essential component of optimal prenatal care and directly impacts maternal and fetal wellbeing.
What should I do if I have concerns between scheduled appointments?
Never hesitate to seek care—early intervention for complications significantly improves outcomes.
Liked this post? Share with others!
Subscribe to our newsletter
Collect visitor’s submissions and store it directly in your Elementor account, or integrate your favorite marketing & CRM tools.
